What It’s Like Living With Endometriosis
Do you have even the slightest idea of what it’s like living with endometriosis? No? Then you’re either a man or you’re a woman who happens to be very lucky. This condition can cause extreme discomfort and severe pain. Worse, it can even prevent women from getting pregnant!
Author:Xander OddityReviewer:Dr. Felix ChaosphereApr 03, 202376 Shares1.4K Views

March is National Endometriosis Month.
We’ve all heard it before. “She’s on the blob.” “It’s that time of the month.” “Riding the red wave.”
There are many stupid names for a monthly bodily function experienced by a large percentage of the human population.
So, why are so many of us expected to put up with such pain?
I was 11 years old when I first went to the doctor about the twice-monthly agony I was in.
I went back and forth, and every time experienced a rushed appointment, an overt lack of sympathy, and endless excuses.

Understanding pain and endometriosis
On one occasion, a doctor even laughed and said it was just an 11-year-old’s overactive imagination. However, this was no laughing matter for me.
Every two weeks, I was then bleeding for two weeks. It was like clockwork: two weeks on, two weeks off.
This was not just “bad period pain.” It was ruining my life.
Anemia followed due to the amount of blood lost each month, and periods were so heavy I couldn’t use tampons.
I remember fellow 12-year-old girls being petrified that this was what their periods would be like too, as I’d accidentally traumatized my year group as one of the first to start.
My schoolbag constantly had night-time sanitary towels in, as that was the only thing that could cope with how heavy my periods were.
What Is Endometriosis?
To try and put it simply, endometriosis is what happens where the cells similar to the ones in the lining of the womb, form elsewhere in the body instead.
Every month, these cells build up and then break down and bleed, just like the uterus cells do.
However, the cells in the womb can leave the body as a period, but this blood has no way to escape. This leads to immense pain, scar tissue forming (called adhesions) and general discomfort.
It can cause painful or heavy periods, and may also lead to infertility, fatigue and bowel and bladder problems.
According to the charity Endometriosis UK, one in ten women suffer from this condition.
That’s over 1.5 million women in the U.K. living with endometriosis.
So, why is so little done about it, or acknowledged by the medical profession?

A Long Wait
As mentioned above, I was 11 when I first went to the doctors for help.
I didn’t get a formal diagnosis until I was 24 - 13 years later. That was ten years ago, and sadly it doesn’t seem like much has changed since.
Recent data found that there’s an average wait of eight years between women first seeing a doctor and receiving a diagnosis.
That’s a long time to live in pain.
The condition can be hereditary, and my mom had suffered with it, too; yet, no doctor would listen or even consider it.
In those 13 years, I was repeatedly fobbed off and told that it was typical teenage periods, that things would settle, and just to wait and see.

I was put on pill after pill, the mini-pill, the full pill, a progesterone-only pill (that made me bleed constantly for six months - fun!).
It wasn’t until I moved to London and found a new female doctor that someone finally accepted it might be endometriosis.
“„Can you believe that average diagnosis time for #endometriosis hasn't changed in a decade? This has to change.- Endometriosis UK
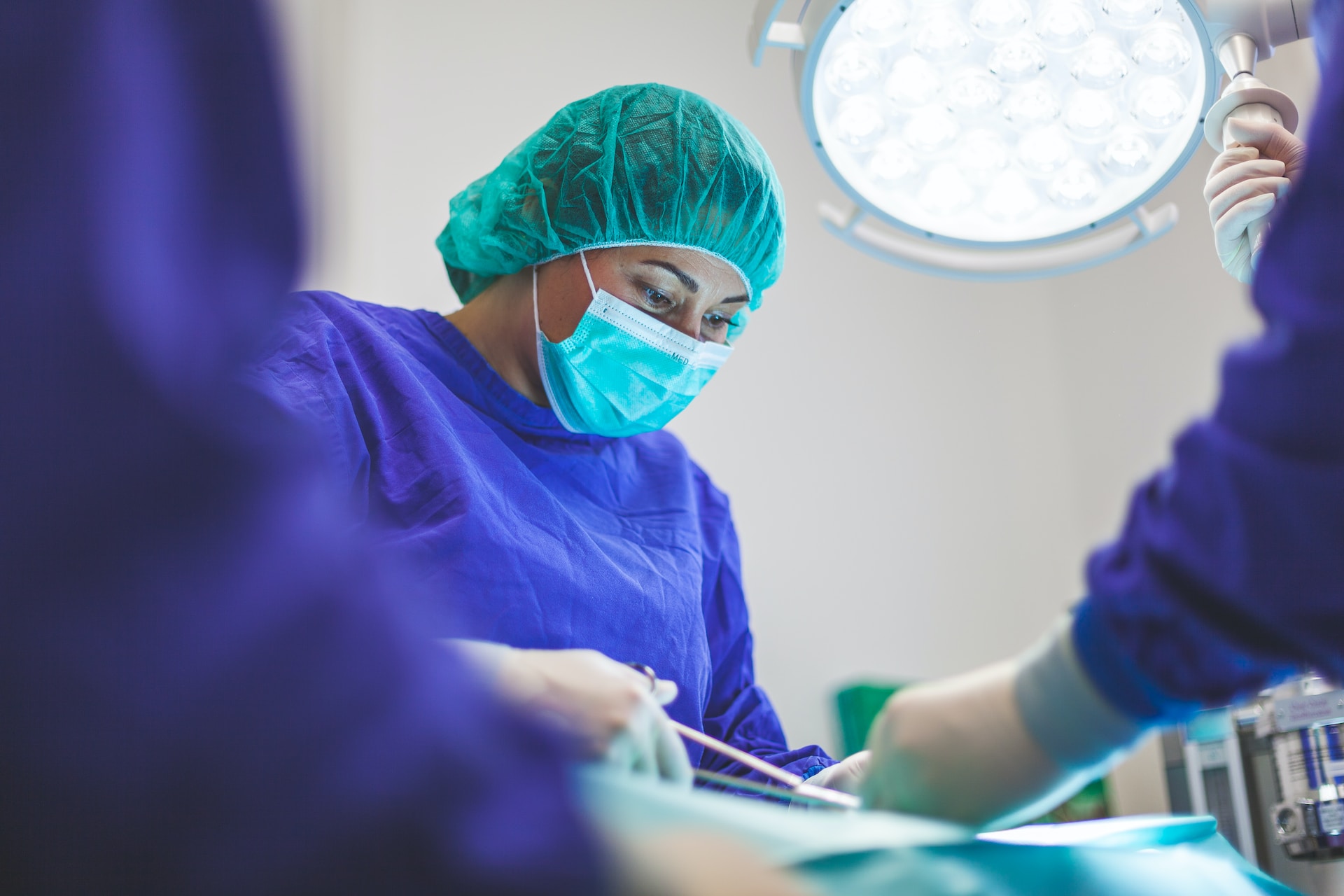
Surgery
The relief after 13 years of being ignored was unreal.
That was the start of a multitude of tests.
All nerves and shyness go out the window for repeated internal examinations, internal ultrasounds (with a wand going exactly where you think it does) before finally being referred for a laparoscopy.
Laparoscopies are the only way endometriosis can be definitively diagnosed, and they involve a camera going into your stomach to have a look around.
It’s usually done by keyhole surgery through or near the navel. The surgeon will use the camera to look around the pelvis to look for the cells that have formed elsewhere.
In my case, they (unsurprisingly to me) found it everywhere, along with a lot of scarring and adhesions.
One of my ovaries had “fused” to the back wall of my pelvis with scar tissue, while the other had a baseball-sized cyst.
All-in-all, it was a fun day for the doctor.
Again, one of the biggest things for me was the reliefthat it hadn’t all been in my head - the pain was real, I had a condition, and all of the pestering and chasing for diagnosis had been worth it.
The Aftermath
Cysts are also surprisingly common with endometriosis.
It was removed and the ovary was retrieved, but the doctor helpfully told me that if I wanted children I should “start and finish my family by 30,” and warned it would probably be difficult.
Another doctor at a later date cheerfully suggested that I just “have a baby” to help the endometriosis, as some women find it lessens after childbirth.
It seems I’m not alone, and women are still being given this decidedly dodgy advice even now.
London-based journalist and BBC broadcaster Emma Barnett (@Emmabarnett) tweeted on March 6, 2021:
“„So many levels of wrong. Also horribly and painfully ironic because of #endometriosis’s horrendous impact on fertility. Hoping this “advice” is ceases immediately. That would ease symptoms of frustration and upset. #EndometriosisAwarenessMonth- Emma Barnett
The diagnosis at least meant I had an answer finally, but it wasn’t the end.
Sadly, endometriosis is incurable, and for many women is a lifelong condition.
Since that first laparoscopy, I had another four years later to remove yet more scar tissue, and that time my OTHER ovary had got stuck somewhere else.
No joke - it’s medically referred to as a “wandering ovary.”
Not quite as fun as a hobbit going for a long walk, but it’s entertaining to imagine.
This second surgery and damage to my second ovary means that the chances of conceiving naturally are next to none - and at 34, I’ve decided I don’t want children anyway.

Painful periods: Living with Endometriosis - BBC London
Contraception
Like me, many women are just prescribed the pill and told to make do.
It wasn’t until my first laparoscopy that someone mentioned the IUD, in this case, the Mirena coil.
It’s an intrauterine device - and it looks like a little plastic “T” shape.
It’s usually only prescribed to women once they’ve had children, hence nobody had mentioned it to me before then.
Having it fitted isn’t the most comfortable experience, but it pales in comparison to the pain I’d suffered from endometriosis.
Within days of having it fitted, the pain eased, and my periods stopped entirely.
To say it’s changed my life would be an understatement.
It can last for up to five years before being replaced. I’ve had a few now and wouldn’t be without it.
Outside of sterilization, the IUD is the most effective type of contraception available, and more successful than the pill. The fact it helped with my endometriosis was an unexpected bonus.
Final Thoughts
So, what can be done to help?
Endometriosis UK are campaigning to #EndoTheStigma.
For National Endometriosis Month, they’re hoping to raise funds and awareness, with a 1 in 10 Challenge.
If you recognize any of my experience, there’s plenty of advice and information on their website too about the next steps you can take.
By knowing what it’s like living with endometriosis, people can raise awareness about this life-altering medical condition.

Xander Oddity
Author
Xander Oddity, an eccentric and intrepid news reporter, is a master of unearthing the strange and bizarre. With an insatiable curiosity for the unconventional, Xander ventures into the depths of the unknown, fearlessly pursuing stories that defy conventional explanation. Armed with a vast reservoir of knowledge and experience in the realm of conspiracies, Xander is a seasoned investigator of the extraordinary.
Throughout his illustrious career, Xander has built a reputation for delving into the shadows of secrecy and unraveling the enigmatic. With an unyielding determination and an unwavering belief in the power of the bizarre, Xander strives to shed light on the unexplained and challenge the boundaries of conventional wisdom. In his pursuit of the truth, Xander continues to inspire others to question the world around them and embrace the unexpected.

Dr. Felix Chaosphere
Reviewer
Dr. Felix Chaosphere, a renowned and eccentric psychiatrist, is a master of unraveling the complexities of the human mind. With his wild and untamed hair, he embodies the essence of a brilliant but unconventional thinker. As a sexologist, he fearlessly delves into the depths of human desire and intimacy, unearthing hidden truths and challenging societal norms.
Beyond his professional expertise, Dr. Chaosphere is also a celebrated author, renowned for his provocative and thought-provoking literary works. His written words mirror the enigmatic nature of his persona, inviting readers to explore the labyrinthine corridors of the human psyche.
With his indomitable spirit and insatiable curiosity, Dr. Chaosphere continues to push boundaries, challenging society's preconceived notions and inspiring others to embrace their own inner tumult.
Latest Articles
Popular Articles