‘Dinner Plate Sized’ Medical Tool Found Inside Woman’s Abdomen Months After Cesarean Birth
In a medical anomaly that has left the world baffled, a ‘dinner plate sized’ medical tool found inside woman’s abdomen months after cesarean birth. This object, described as being 'dinner plate-sized,' turned out to be an Alexis wound retractor (AWR), a surgical instrument typically used to maintain wound access during abdominal surgeries.
Author:Maxwell CanvasReviewer:Scarlet SunsetSep 06, 202317.9K Shares365.5K Views
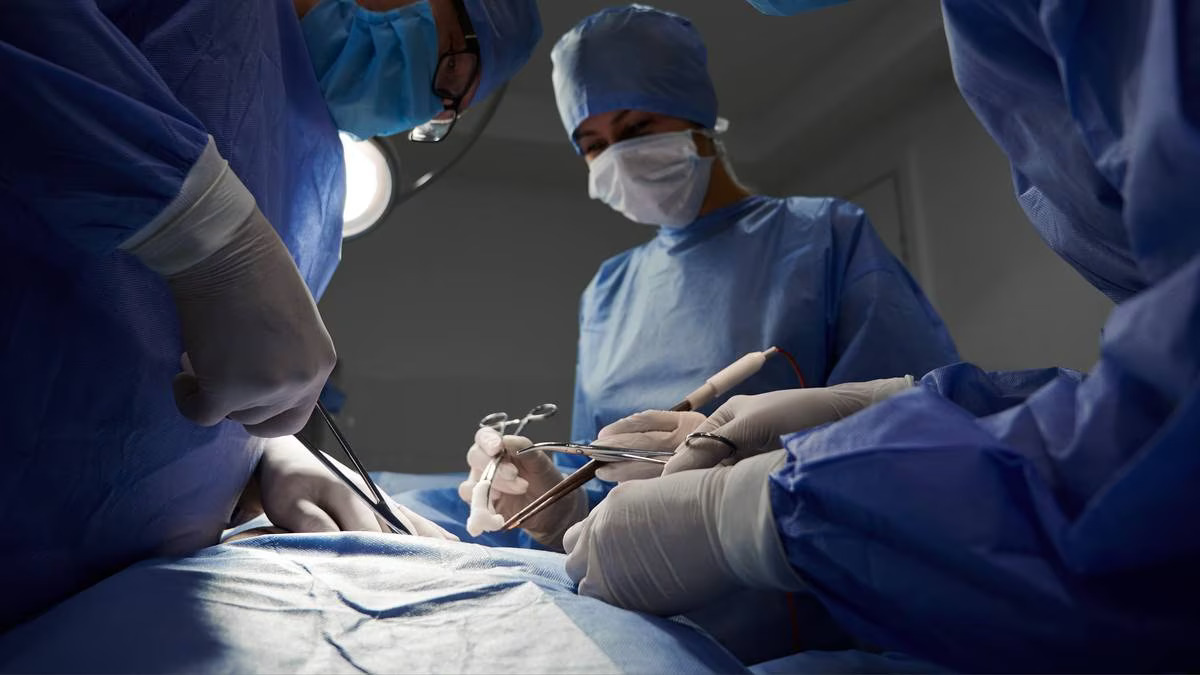
In a medical anomaly that has left the world baffled, a ‘dinner plate sized’ medical tool found inside woman’s abdomen months after cesarean birth. This object, described as being 'dinner plate-sized,' turned out to be an Alexis wound retractor (AWR), a surgical instrument typically used to maintain wound access during abdominal surgeries. This extraordinary incident has sparked discussions surrounding patient safety, surgical protocols, and the resilience of the human body.
In the realm of modern medicine, surgical protocols stand as a testament to the commitment of healthcare professionals to patient safety and well-being. These protocols serve as a guiding framework that ensures that surgeries, whether routine or complex, are conducted with the highest levels of expertise, precision, and care.
Patient well-being remains at the core of surgical protocols, drivingcontinual advancements in medical practices to provide patients with the best possible outcomes and experiences.
Surgical Instrument Discovered Inside Woman's Abdomen
According to a studyby New Zealand's Health and Disability Commissioner, a ‘dinner plate sized’ medical tool found inside woman’s abdomen months after cesarean birth in New Zealand.
According to officials, a surgeon, a senior registrar, an instrument nurse, three circulating nurses, two anesthetists, two anesthetic technicians, and a theater midwife were among the numerous operating room theater professionals who attended the C-section at the time of the procedure.
Following the mother's delivery of her child at Auckland City Hospital in 2020, an Alexis retractor, or AWR, which can measure 17 centimeters (6 inches) in diameter, was left inside the mother's body.
The AWR is a retractable cylindrical tool with a translucent film that is used in surgery to pull back the borders of a wound.
The woman, however, soon started experiencing significant abdominal pain and started mentioning it to her doctor "a number of times in the 18 months after the C-section," including one occasion when she visited the emergency room at Auckland City Hospital due to the pains being so bad.
The woman underwent many tests to determine what was wrong after experiencing severe pain for months, including X-rays, which revealed no evidence of the device. When the discomfort became unbearable, she went to the hospital's emergency room. A CT scan of her abdomen revealed the device, which was promptly removed in 2021.
The object was missed for so long in part because it was "non-radio opaque" and therefore invisible to x-rays.
According to McDowell, the Auckland health authority failed in its responsibility to take care of the woman. The health board has expressed regret for the upset it has brought about, but it must do so once more in writing within three weeks.
Te Whatu Ora Auckland, the Auckland District Health Board, was found to have violated the code of patient rights, according to a report released on Monday (September 4) by New Zealand's Health and Disability Commissioner, Morag McDowell.
The health board initially asserted that a nurse, in her 20s, caring for the woman during the cesarean, had not shown the patient reasonable skill and care.
McDowell said:
“„I acknowledge the stress that these events caused to the woman and her family. The woman experienced episodes of pain over a significant period of time following her surgery until the AWR was removed in 2021. I accept her concerns regarding the impact this had on her health and wellbeing and that of her family. As set out in my report, the care fell significantly below the appropriate standard in this case and resulted in a prolonged period of distress for the woman. Systems should have been in place to prevent this from occurring.- Morag McDowell
According to the report, a large wound retractor was utilized during the C-section procedure, but the surgeon thought it was too small and requested an extra-large model. When a CT scan was performed more than a year later, it was this second, larger device that had been left inside the patient.
The placenta previa condition, which occurs when the placenta totally or partially covers the opening of the uterus during pregnancy, prompted the woman to have a scheduled C-section, according to the study.
The AWR was not included in a tally of all surgical tools used during the operation in 2020, according to the commission report. According to a nurse who testified before the committee, this may be "because the Alexis Retractor does not go into the wound completely as half of the retractor needs to remain outside the patient and so it would not be at risk of being retained."
McDowell suggested that the Auckland District Health Board amend its policy to include AWRs as part of the surgical count and issue a formal written apology to the woman.
The director of proceedings has also been tasked with reviewing the case to determine whether any additional action is necessary.
Te Toka Tumai Auckland's group director of operations at Te Whatu Ora Health New Zealand, Dr. Mike Shepherd, issued an official statement apologizing for the blunder.
“„On behalf of our Women’s Health service at Te Toka Tumai Auckland and Te Whatu Ora, I would like to say how sorry we are for what happened to the patient, and acknowledge the impact that this will have had on her and her whānau [family group]. We would like to assure the public that incidents like these are extremely rare, and we remain confident in the quality of our surgical and maternity care.- Dr. Mike Shepherd
The Implications For Patient Safety
This discovery raises critical questions about patient safety and surgical protocols. How did an instrument as substantial as an AWR device go unnoticed within the patient's body for over a year? What safeguards should be in place to prevent such occurrences? These questions underscore the need for thorough and systematic counting of surgical instruments and comprehensive post-operative checks.
The Resilience Of The Human Body
Remarkably, despite the presence of this sizable foreign object, the woman did not experience severe health complications. This case showcases the extraordinary resilience of the human body, which can adapt to unexpected circumstances. However, it also emphasizes the importance of timely medical interventions and regular check-ups to ensure the well-being of patients.
Calls For Enhanced Protocols
This incident has prompted discussions within the medical community regarding the need for enhanced surgical protocols. Stringent instrument counting procedures, advanced imaging technologies, and meticulous post-operative monitoring are among the measures being considered to prevent similar oversights in the future.
The Importance Of Patient Advocacy
This case underscores the significance of patient advocacy and empowerment. Patients are encouraged to actively engage in their healthcare, ask questions, and seek second opinions when necessary. While medical professionals strive to provide the best care, patients play a crucial role in safeguarding their own well-being.
Surgical Protocols And Patient Well-being
Surgical protocols are a vital component of modern healthcare, playing a central role in ensuring patient safety, minimizing risks, and promoting successful outcomes. These protocols encompass a wide range of procedures and guidelines that medical professionals follow before, during, and after surgery. In this detailed exploration, we delve into the importance of surgical protocols and their direct impact on patient well-being.
The Foundation Of Surgical Protocols
Surgical protocols are established sets of standardized procedures and practices designed to enhance the safety and effectiveness of surgical interventions. These protocols are developed and refined through extensive research, clinical experience, and the collective wisdom of healthcare professionals. They serve as a foundation for consistent and high-quality patient care.
Preoperative Assessment And Planning
One of the initial steps in surgical protocols is the preoperative assessment and planning phase. This involves a thorough evaluation of the patient's medical history, current health status, and any pre-existing conditions. This assessment is crucial for identifying potential risks and complications that could affect the surgery.
During this phase, surgical teams also engage in meticulous planning. This includes selecting the appropriate surgical approach, coordinating the anesthesia plan, and ensuring the availability of necessary equipment and resources. Proper planning sets the stage for a smooth and well-executed procedure.
Informed Consent
Informed consent is a fundamental aspect of surgical protocols and patient rights. Medical professionals are required to obtain the patient's informed and voluntary consent before performing any surgery. This process involves explaining the procedure, potential risks, benefits, and available alternatives to the patient. Informed consent ensures that patients have a say in their treatment and are aware of what to expect.
Sterile Environment
Maintaining a sterile surgical environment is paramount in preventing infections and complications. Surgical teams follow strict protocols to ensure the operating room (OR) is aseptic. This includes thorough handwashing, the use of sterile gowns and gloves, and the sterilization of surgical instruments. The goal is to minimize the risk of surgical site infections that can have serious consequences for patients.
Patient Safety During Surgery
During surgery, patient safety remains a top priority. Anesthesia protocols are carefully managed to ensure patients are in a controlled and comfortable state. Surgical teams follow strict protocols for instrument handling, suturing, and wound closure to minimize the risk of errors and complications.
In addition to monitoring the patient's vital signs, surgical teams also employ advanced technologies and monitoring devices to track various physiological parameters in real-time. This proactive approach allows for immediate intervention should any irregularities arise during the procedure.
Postoperative Care And Recovery
Surgical protocols extend beyond the operating room and into the postoperative phase. Proper postoperative care is crucial for monitoring patient recovery and preventing complications. Protocols include regular monitoring of vital signs, pain management, wound care, and infection prevention measures.
Patients are provided with clear postoperative instructions to follow during their recovery period. This includes guidance on medication, dietary restrictions, and physical activity. Surgical teams remain accessible to address any concerns or complications that may arise during the recovery process.
Continual Advancements And Adaptations
Surgical protocols are not static; they evolve in response to emerging medical knowledge, technological advancements, and changing patient demographics. Medical professionals continually update their practices to incorporate the latest evidence-based guidelines and best practices.
The Role Of Communication
Effective communication among members of the surgical team is a cornerstone of successful surgical protocols. Surgeons, nurses, anesthesiologists, and other healthcare providers must collaborate seamlessly to ensure patient safety. Briefings, checklists, and debriefings are often employed to enhance communication and reduce the risk of errors.
Reducing Surgical Complications
One of the primary goals of surgical protocols is to minimize the risk of complications. This includes not only surgical site infections but also complications related to anesthesia, blood clot formation, and adverse reactions to medications. By following established protocols, medical professionals can significantly reduce the likelihood of adverse events.
The Impact On Patient Well-Being
The meticulous adherence to surgical protocols has a direct and profound impact on patient well-being. Patients who undergo surgical procedures benefit from a higher level of safety, reduced complications, and improved outcomes. Moreover, the psychological well-being of patients is positively influenced when they have confidence in the healthcare system's commitment to their safety.
Challenges And Ongoing Improvements
While surgical protocols have come a long way in ensuring patient safety, challenges persist. These include issues such as surgical errors, communication breakdowns, and disparities in healthcare access. Healthcare organizations continue to work diligently to address these challenges and improve the overall quality of surgical care.
People Also Ask
What Is The Incident Of The 'Dinner Plate-sized' Device Found Inside A Woman's Abdomen 18 Months After A Cesarean Birth?
In a medical anomaly, a woman in New Zealand discovered a 'dinner plate-sized' surgical instrument inside her abdomen 18 months after her Cesarean section.
What Type Of Surgical Instrument Was Found Inside The Woman's Abdomen?
The foreign object found inside the woman's abdomen was identified as an Alexis wound retractor (AWR), a surgical instrument used in abdominal procedures.
What Implications Does This Case Have For Patient Safety And Surgical Protocols?
This case raises important questions about patient safety and surgical protocols, highlighting the need for meticulous instrument counting and post-operative checks to prevent such incidents.
How Was The Foreign Object Removed From The Woman's Abdomen?
The woman underwent a surgical procedure to successfully remove the Alexis wound retractor (AWR) device from her abdomen.
What Are The Implications Of This Case For The Ongoing Discussions About Patient Safety And Healthcare Excellence?
This case serves as a catalyst for ongoing discussions within the medical community regarding patient safety, medical oversight, and the continuous pursuit of excellence in healthcare delivery.
Conclusion
A ‘dinner plate sized’ medical tool found inside a woman’s abdomen months after cesarean birth. This is a stark reminder of the complexities of modern healthcare. It highlights the need for meticulous surgical protocols, stringent instrument counts, and comprehensive post-operative monitoring to prevent such oversights. While this case is a rarity, it serves as a compelling catalyst for ongoing discussions about patient safety, medical oversight, and the relentless pursuit of excellence in healthcare delivery.

Maxwell Canvas
Author
Maxwell Canvas, a charismatic and fearless crypto evangelist, defies conventions and blazes a trail in the realm of digital currencies. With his unique physique serving as a symbol of resilience, he challenges societal norms and proves that true expertise transcends appearances. Against a backdrop of a blurred and ever-shifting market, Maxwell's work becomes a masterpiece, painting a vivid picture of knowledge and inspiration.
With unwavering passion, Maxwell empowers others to embrace the transformative potential of blockchain technology. His captivating presence and unyielding dedication captivate audiences, turning skepticism into curiosity and igniting a spark of interest in the world of cryptocurrencies. Maxwell Canvas stands as a visionary force, leaving an indelible mark on the crypto landscape, inspiring others to explore decentralized possibilities and embrace a future of innovation and financial empowerment.

Scarlet Sunset
Reviewer
Scarlet Sunset is a captivating and confident transgender individual who radiates sensuality and embraces her unique beauty. With a radiant smile and a touch of red lipstick, she captivates hearts by the poolside as the sun dips below the horizon, casting a warm glow on her unforgettable presence.
Despite societal norms and expectations, Scarlet celebrates her body, proudly defying conventional standards of beauty. Her curves tell a story of self-acceptance and empowerment, challenging stereotypes and inspiring others to embrace their own bodies without reservation.
Latest Articles
Popular Articles

